Overdose isn’t just a street drug problem. It happens every day to people taking prescribed medications the wrong way - especially when those meds come in patch, liquid, or extended-release forms. These aren’t ordinary pills. They’re designed to release medicine slowly, stick to your skin, or dissolve in your mouth. But if you don’t use them exactly as directed, they can kill you - fast.
Why These Forms Are Riskier Than Regular Pills
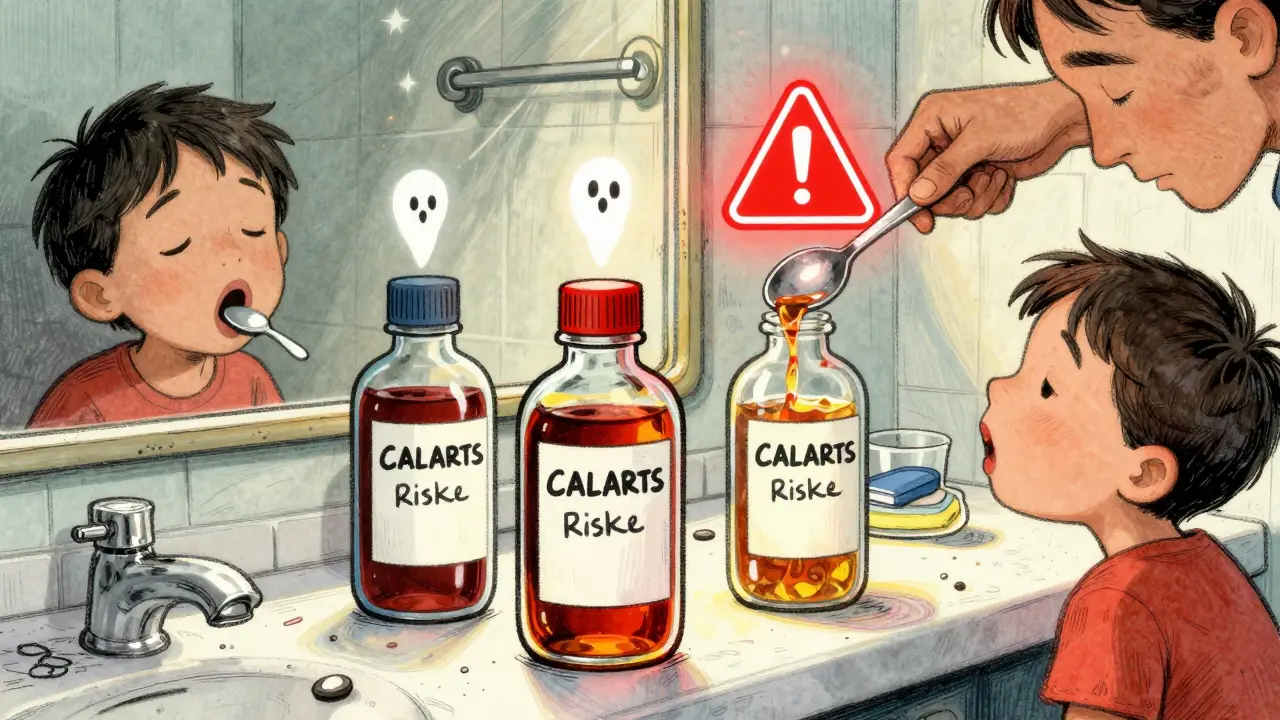
Think of a regular tablet. You swallow it. It breaks down in your stomach. The drug enters your system slowly. Now imagine a fentanyl patch. It’s stuck to your skin. It’s meant to deliver a steady dose over 72 hours. But if you cut it open, heat it with a hair dryer, or wear two at once? You’re not getting pain relief. You’re getting a lethal rush of opioid into your bloodstream. Liquid medications - like morphine syrup or cough medicine with codeine - are even trickier. A teaspoon isn’t the same as a tablespoon. A plastic spoon from your kitchen? It’s not calibrated. One wrong scoop, and you’ve taken three times your dose. And because these liquids often come in similar-looking bottles, mixing them up is easy. One person thought they were taking their headache medicine. It was their son’s ADHD medication. He ended up in the ER. Extended-release pills - like OxyContin, Vyvanse, or long-acting oxycodone - are made to last. But if you crush, chew, or dissolve them? All the drug hits your system at once. That’s like taking 10 regular pills in one go. In 2023, over 2,700 overdose deaths in the U.S. involved extended-release opioids, according to CDC data. Most of those happened because someone didn’t understand how the pill worked.How to Use Patches Safely
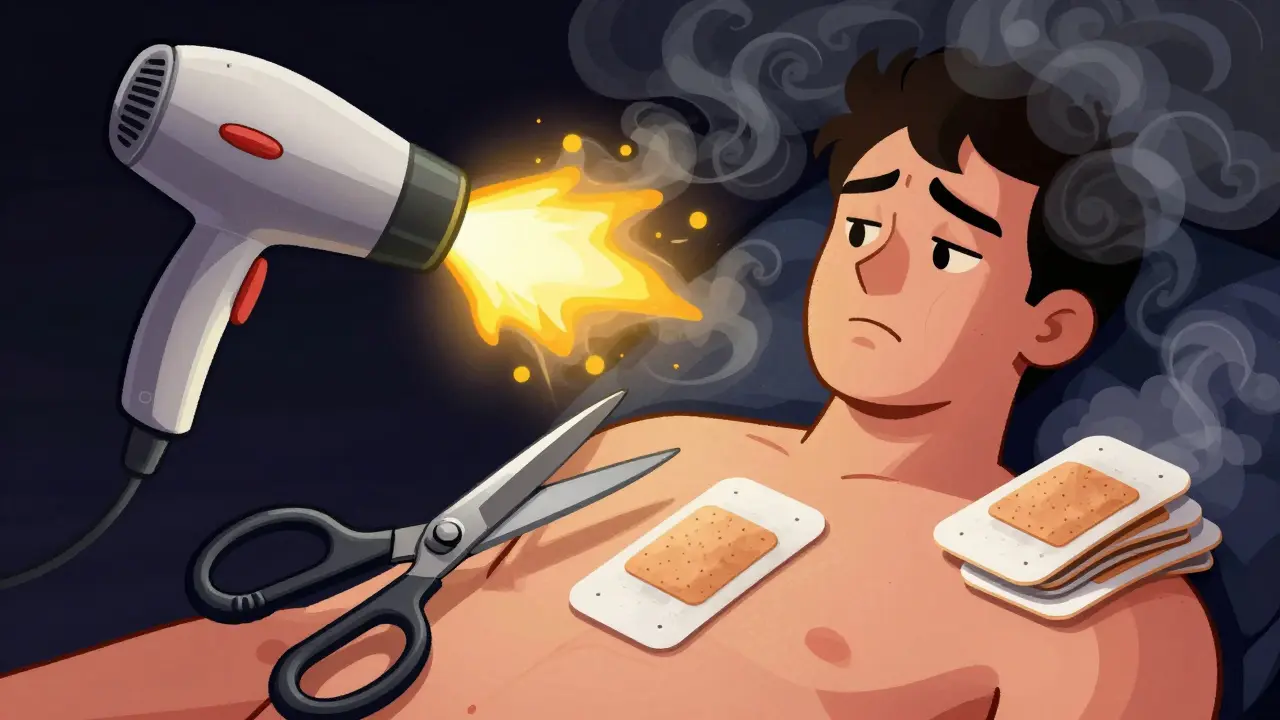
Fentanyl, buprenorphine, and nicotine patches are common. Here’s how to avoid danger:- Never cut, chew, or heat the patch. Heat - from a heating pad, hot bath, or even sunbathing - makes the drug release too fast. People have died from this.
- Apply it to clean, dry skin. No lotions, oils, or alcohol on the spot. That changes how the drug is absorbed.
- Use one patch at a time. Never stack them. Even if your pain feels worse, adding another patch won’t help - it’ll kill you.
- Dispose of used patches safely. Fold the sticky side over itself. Flush it down the toilet or take it to a drug take-back site. Kids or pets can overdose from just touching a used patch.
- Don’t share patches. A patch meant for a 200-pound adult could kill a 120-pound person. This isn’t theoretical. In 2022, a teenager died after wearing a parent’s fentanyl patch.
How to Use Liquid Medications Safely
Liquid meds are often used for kids, elderly people, or those who can’t swallow pills. But they’re easy to mess up.- Always use the dosing tool that came with the bottle. A cap, spoon, or syringe from another medicine? It’s not accurate. A syringe marked in milliliters (mL) is best. Never use a kitchen spoon.
- Double-check the concentration. Some liquid opioids come as 5 mg per 5 mL. Others are 10 mg per 5 mL. Mixing them up is deadly. Write the concentration on the bottle with a marker.
- Keep liquids locked up. Children have mistaken opioid syrups for candy or juice. Store them in a locked cabinet - not just out of reach.
- Don’t mix with alcohol or sleep aids. Liquid opioids + alcohol = slowed breathing. Liquid opioids + benzodiazepines = high chance of stopping breathing. This combo kills more people than any single drug.
- Write down your dose. If you’re giving meds to someone else, write: “Take 2 mL at 8 a.m. and 8 p.m.” Put it on the fridge. People forget. Especially when they’re tired or in pain.
How to Use Extended-Release Medications Safely
These are the most dangerous if misused. They’re made to last 8, 12, or even 24 hours. But that design can turn into a trap.- Never crush, break, or chew these pills. Ever. If you can’t swallow it whole, talk to your doctor. There are other forms - patches, liquids, or immediate-release versions - that might work better.
- Take it exactly on schedule. Skipping a dose? Don’t double up later. Taking two at once can cause overdose. If you miss a dose, call your prescriber. Don’t guess.
- Watch for signs of too much. Slurred speech, slow breathing, blue lips, or passing out? That’s overdose. Call 911. Don’t wait.
- Don’t combine with other depressants. Alcohol, sleeping pills, muscle relaxers, or even some anxiety meds? They all slow your breathing. Add them to an extended-release opioid? You’re playing Russian roulette.
- Know your dose. If your doctor changes your dose, ask: “Is this still extended-release?” Sometimes, a pill looks the same but isn’t. A switch from 30 mg extended-release to 30 mg immediate-release can be fatal if you’re used to the slow release.
Naloxone: Your Lifeline - But Not a Cure-All
Naloxone (Narcan) saves lives. It reverses opioid overdoses. But here’s what no one tells you:- It wears off. Naloxone lasts 30 to 90 minutes. Fentanyl patches and extended-release pills keep releasing opioid for hours. That means after naloxone wears off, the person can slip back into overdose. You must get them to a hospital - even if they seem fine.
- One dose isn’t always enough. Fentanyl is so strong that sometimes you need two or three doses of naloxone. Keep extra kits handy.
- It doesn’t work on non-opioid drugs. If someone overdoses on cocaine, benzodiazepines, or meth, naloxone won’t help. But if you’re unsure - give it anyway. It’s safe. And it might save them.
Keep naloxone in your wallet, car, or medicine cabinet. You don’t need a prescription in most states. Ask your pharmacist. Get trained. Practice with a training kit. You don’t need to be a nurse. You just need to be ready.

What to Do If Someone Overdoses
If someone is unresponsive, not breathing, or turning blue:- Call 911 immediately. Say: “They’re not waking up. I think they overdosed.”
- Give naloxone. Spray one dose into one nostril. If no response in 3 minutes, give a second dose.
- Start chest compressions if they’re not breathing. Push hard and fast on the center of the chest.
- Stay with them. Even if they wake up, don’t let them go to sleep. Keep them awake until EMS arrives.
And here’s the most important part: Call 911 even if you give naloxone. Many people are afraid of legal trouble. In 49 states, the Good Samaritan Law protects you if you call for help during an overdose. You won’t get arrested. The person won’t get arrested. You’re saving a life.
What You Can Do Right Now
- Check your medicine cabinet. Are there old patches? Unused liquids? Expired extended-release pills? Take them to a drug take-back location. Don’t flush them unless the label says to.
- Ask your doctor: “Is this medication extended-release? What happens if I miss a dose? Can I switch to something safer?”
- Get naloxone. It’s free or low-cost at pharmacies, community centers, and health departments. Keep one at home. Keep one in your car.
- Teach someone. Show a friend or family member how to use naloxone. Give them a kit. You never know who might need it tomorrow.
Overdose isn’t about being careless. It’s about not knowing. These medications are powerful. They help people live. But they can kill - if you don’t treat them with the respect they demand. You don’t need to be an expert. Just be informed. Be prepared. And be ready to act.
Can I use a fentanyl patch if I’ve never taken opioids before?
No. Fentanyl patches are only for people already used to strong opioids. If you’ve never taken opioids, your body can’t handle the steady dose. It can cause breathing to stop. Doctors only prescribe patches to patients who have been on lower-dose opioids for at least a week.
Is it safe to store liquid opioids in the fridge?
Some liquid opioids need refrigeration - check the label. But others shouldn’t be chilled. Cold can change how the medicine works. If the bottle doesn’t say to refrigerate, keep it at room temperature. Always store it in a locked container, no matter where you keep it.
What if I accidentally crush an extended-release pill?
Don’t take it. Throw it away. Wash your hands. Call your doctor or pharmacist. Even if you only took a small piece, the dose you just got may be 3 to 5 times higher than normal. Go to the ER. Don’t wait for symptoms.
Can naloxone be used on children who overdose on liquid opioids?
Yes. Naloxone works the same in children and adults. If a child overdoses on liquid opioids, give naloxone right away. Call 911. Even if they wake up, they still need medical care. Children’s bodies process drugs differently, and the overdose risk doesn’t go away after one dose of naloxone.
Are there non-opioid alternatives to extended-release pain meds?
Yes. Depending on the condition, options include non-opioid pain relievers like gabapentin, physical therapy, nerve blocks, or even cognitive behavioral therapy. Talk to your doctor about alternatives. You don’t have to stay on opioids if you’re worried about overdose risk.


bill cook
I've been using fentanyl patches for years and honestly? The scariest part isn't the patch itself-it's when your doctor forgets to tell you that heat makes it dump all the drug at once. My cousin died because he took a hot shower after putting on a new patch. No one warned him. No one. Just another statistic.
And don't even get me started on how pharmacies hand out these things like candy. No ID check. No counseling. Just 'here, have fun.' It's not healthcare-it's a waiting room for an autopsy.