Epinephrine Auto-Injector Training Simulator
Emergency Response Protocol Trainer
Follow each step carefully. Real emergencies don't wait.
Step 1: Preparation
Before you can use the auto-injector, you must prepare it correctly.
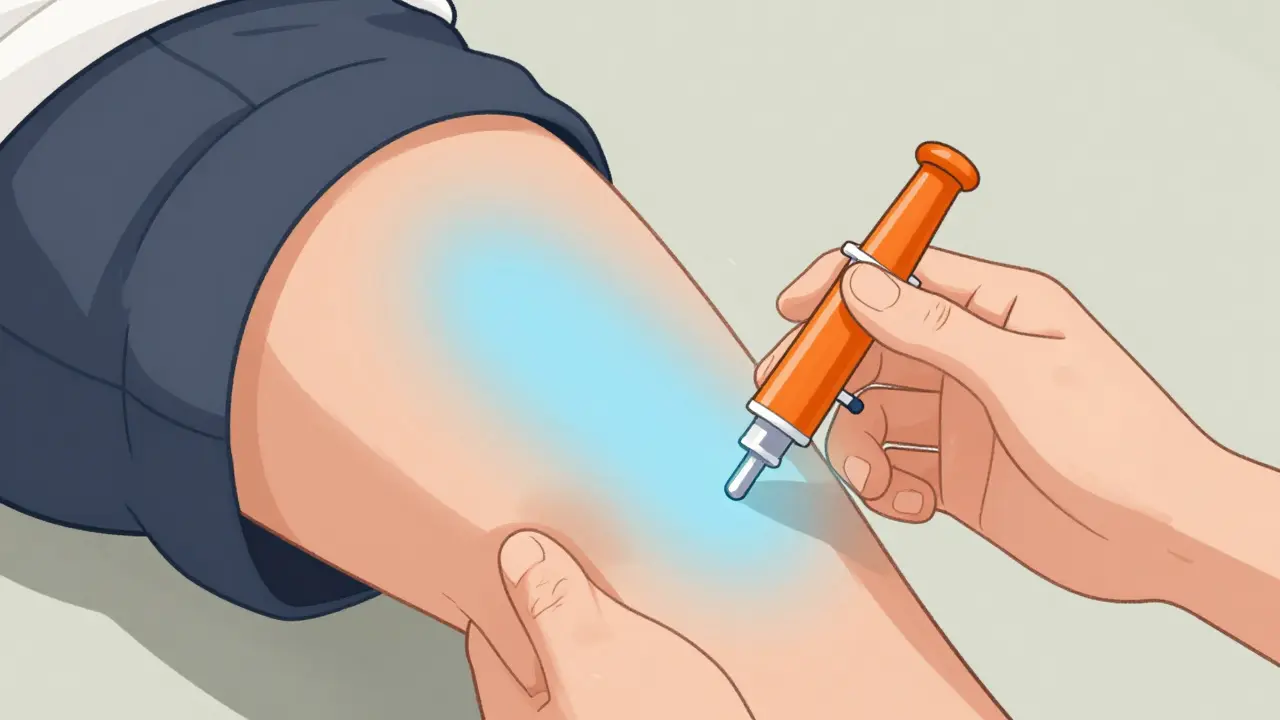
Step 2: Placement
Where you inject matters critically for medication absorption speed.
Step 3: Duration
Holding time varies by brand. Know your specific device.
• AUVI-Q: Hold for 10 seconds
• EpiPen: Hold for 3 seconds
• Always check manufacturer instructions
Step 4: Post-Action Care
Your work isn't done after injection. Monitor closely.
Training Complete!
Remember: Practice makes perfect. Refresh your skills annually.
Critical Reminders:
- Five-minute window is crucial
- Second dose may be needed (16-35% of cases)
- Monitor for biphasic reactions hours later
- Always follow up with medical care
Legal Protection:
Good Samaritan laws protect those acting in good faith during emergencies. Don't let fear delay life-saving treatment.
Every minute counts when someone is having a severe allergic reaction. We often think we have plenty of time to call 911, grab the medicine, and help the person breathe. But studies show survival hinges on getting epinephrine auto-injector into muscle tissue within five minutes. If you wait longer, the odds drop sharply. This isn't just theory; it's the difference between life and death in schools, homes, and workplaces. Proper training turns panic into protocol.
Understanding the Five-Minute Window
The body reacts fast to allergens like peanuts, bee stings, or latex. When anaphylaxis kicks in, blood pressure crashes and airways swell. Research from the American Academy of Allergy, Asthma & Immunology highlights that severe outcomes increase by 44 percent for every minute of delay beyond the initial five minutes. It sounds harsh, but biology doesn't negotiate. Waiting for symptoms to clear before acting is a dangerous gamble. Most fatal cases involve people who thought the reaction was mild initially, only for it to spiral into shock later.
Anaphylaxis is a severe, potentially life-threatening allergic reaction that occurs rapidly after exposure to an allergen. According to data from the Centers for Disease Control and Prevention, approximately 1 in 13 children has a food allergy. With 30 percent of these children having multiple food allergies, the risk is widespread.You cannot manage this risk without knowing exactly what to do. Knowing the device is one thing; knowing how to deploy it under stress is another.
The Mechanics of Correct Administration
Having the injector in your pocket means nothing if you can't use it right. Technical specifications are precise. For adults and students weighing over 66 pounds, you must inject into the lateral (outer) thigh. Not the arm, not the buttocks. The outer thigh allows the medication to reach the bloodstream quickly. If you aim for the front of the leg, absorption slows down, wasting precious time.
Dosage matters too. Standard doses are 0.30 mg for individuals meeting weight criteria, while pediatric versions exist for smaller children. Devices differ in mechanics. Some require removing a blue cap and a green cap; others just need a firm push against the leg. For example, AUVI-Q devices require holding the fist with the blue safety cap up and the needle end down. You must maintain pressure for 10 seconds. Other brands might only need two seconds. Confusion between brands leads to hesitation.
| Action Step | Correct Technique | Common Error |
|---|---|---|
| Preparation | Remove safety caps firmly | Failing to remove protective cover |
| Placement | Lateral (outer) thigh on bare skin | Injecting through pants or into belly |
| Duration | Hold for manufacturer specified time | Releasing too early |
| Post-Action | Cover patient to prevent shock | Leaving patient alone |
Why Training Programs Fail
We assume watching a video is enough. It isn't. Hands-on practice reduces administration errors by 78 percent compared to lecture-only formats. Without physical drills, skill retention drops to 47 percent after just six months. Many schools train staff once a year, but real emergencies don't wait for schedules. Trainers often miss critical details during role-plays. I've seen instructors forget to emphasize injecting on bare skin. Clothes act as a barrier. One teacher tried to inject through denim jeans in a drill because the simulation didn't flag it as wrong.
Another major failure point is fear. Surveys show 42 percent of staff hesitate due to fear of legal repercussions. They worry about being sued if the shot misses or if the child needs more care. Fortunately, Good Samaritan laws exist in most jurisdictions to protect those acting in good faith during medical emergencies. Yet the anxiety remains. Training must address this psychological barrier, not just the physical steps.
Benchmarking Standards and Regulations
Effective training isn't optional; it is often mandated. Look at how different regions enforce this. California's Education Code requires written materials to be kept for three years and specifies monitoring for signs of shock, such as covering the individual with a blanket to maintain body temperature. Illinois mandates a strict two-year validity period for training certificates. These aren't red tape; they ensure knowledge stays fresh.
In Ohio, the system uses OhioTRAIN with a specific Course ID, requiring a video component followed by a post-test. This creates a standardized baseline. While you might be reading this from Melbourne, these rigorous frameworks highlight what works globally. Any competent program should demand competency testing. Simply checking a box isn't enough. Staff must demonstrate psychomotor skills-moving their hands correctly to deliver the dose.
Managing the Second Dose and Aftercare
What happens after the click? About 16 to 35 percent of anaphylaxis cases require a second dose. You must monitor the patient closely. If symptoms continue or worsen five minutes after the first injection, and paramedics haven't arrived, administer a second auto-injector if available. This is where having a stock supply in the school or workplace becomes vital.
Don't forget post-injection care. The patient may go into shock even if breathing improves. Covering them with a blanket helps maintain body temperature. Monitor airway, breathing, and heart rate every five minutes until help arrives. Ignoring biphasic reactions-where symptoms return hours later-is a leading cause of long-term issues. Always insist the patient sees a doctor after any use, even if they feel fine.

Building a Culture of Safety
Schools and organizations are shifting toward integrated systems. Some districts now sync training records with health information systems, reducing expired medication incidents by 94 percent. Technology helps, but culture drives action. Virtual reality modules launched recently reduce training time by 35 percent while improving retention. However, the human element of confidence remains key. You need to feel comfortable picking up the device and trusting your muscles to do the job.
Persistent challenges remain, especially in areas with high staff turnover. Rural districts report difficulties maintaining trained personnel. Refresher courses are non-negotiable. Mandatory annual refreshers are the only way to stop skills from fading. When staff are confident, delays disappear. When they hesitate, patients suffer.
Conclusion and Action Items
Your safety plan is only as strong as the weakest link in the chain. That link is often the person holding the injector. Verify your team knows the device brand specifics. Schedule quarterly practice sessions with trainer devices. Ensure you have enough inventory for potential second doses. Finally, review your protocols annually. Knowledge fades fast; practice keeps it sharp.
How long do I hold the epinephrine auto-injector in place?
Holding times vary by brand. AUVI-Q requires 10 seconds, while some other devices require only 2 to 3 seconds. Always read the specific manufacturer label included with your device and verify during training.
Where is the correct injection site?
Inject into the outer (lateral) mid-thigh. Do not inject through clothing if possible. Remove or pull aside pants to ensure the needle penetrates skin directly.
When should I give a second dose of epinephrine?
If symptoms persist or worsen after 5 minutes of the first injection and emergency services have not yet arrived, administer a second dose. Do not wait for symptoms to resolve before calling for help again.
Is training required for school staff?
Many jurisdictions, including states like California, Illinois, and Ohio, mandate specific training standards for school personnel. Even where not legally required, it is highly recommended for safety plans.
Can I use an expired epinephrine auto-injector?
Ideally, no. Expired devices may not deliver full potency. However, in a life-or-death situation where no other option exists, using an expired auto-injector is better than giving nothing.



Jordan Marx
Physiological response times dictate immediate intervention strategies during anaphylactic events. Proper psychomotor skill acquisition ensures device deployment without hesitation under stress conditions. Muscle memory training bridges the gap between theoretical knowledge and practical execution effectively. The lateral thigh injection site provides optimal vascular absorption rates for rapid pharmacokinetics. Delayed administration correlates directly with adverse outcomes in documented case studies. Staff competency verification remains the single most critical control point in emergency protocols. Standardized equipment familiarity reduces cognitive load during high-stress incidents significantly. Regulatory frameworks mandate specific intervals for recertification to prevent skill decay over time. Inventory management systems track expiration dates to maintain operational readiness standards. Secondary dosing requirements highlight the importance of maintaining adequate supply chains. Clinical oversight confirms the necessity of monitoring biphasic reactions post-intervention. Healthcare providers emphasize that fabric barriers impede needle penetration speed considerably. Emergency response teams prioritize airway stabilization alongside vasoactive drug delivery. Institutional culture influences individual willingness to act without external permission or guidance. Liability protections exist to shield good actors who attempt life-saving measures correctly. Ongoing education refreshes memory retention regarding brand-specific mechanical variations. Simulation environments allow safe failure identification before real world application scenarios. Ultimately the margin for error disappears once symptoms manifest visibly.